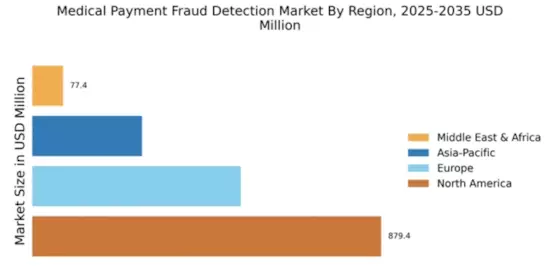
Market Growth Projections
The Global Medical Payment Fraud Detection Market Industry is projected to experience substantial growth in the coming years. The market is expected to reach a valuation of 1.76 USD Billion in 2024 and is anticipated to expand to 14.7 USD Billion by 2035. This growth trajectory suggests a compound annual growth rate (CAGR) of 21.29% from 2025 to 2035. Such projections indicate a robust demand for innovative fraud detection solutions as healthcare organizations seek to combat the rising tide of fraudulent activities. The increasing complexity of healthcare billing and the need for compliance with regulatory standards further contribute to this market expansion.
Rising Healthcare Expenditure
Rising healthcare expenditure is a substantial factor influencing the Global Medical Payment Fraud Detection Market Industry. As global healthcare spending continues to increase, the potential for fraud also escalates. With healthcare costs projected to rise significantly, the financial stakes associated with fraudulent claims become more pronounced. This scenario compels healthcare providers and insurers to adopt advanced fraud detection mechanisms to protect their financial interests. The market's growth trajectory, with an expected value of 14.7 USD Billion by 2035, indicates that stakeholders are increasingly prioritizing investments in fraud detection technologies to mitigate risks associated with rising expenditures.
Growing Awareness Among Stakeholders
Growing awareness among stakeholders regarding the impact of medical payment fraud is a significant driver for the Global Medical Payment Fraud Detection Market Industry. Healthcare providers, insurers, and patients are increasingly recognizing the detrimental effects of fraud on healthcare systems. This heightened awareness is prompting stakeholders to seek out effective fraud detection solutions to protect their interests. As a result, investments in fraud detection technologies are on the rise, with healthcare organizations prioritizing the implementation of systems that can safeguard against fraudulent activities. This trend is expected to contribute to the market's robust growth in the coming years.
Increasing Incidence of Fraudulent Claims
The rising incidence of fraudulent claims is a primary driver for the Global Medical Payment Fraud Detection Market Industry. As healthcare costs escalate, fraudulent activities such as billing for services not rendered or upcoding have become more prevalent. In 2024, the market is valued at 1.76 USD Billion, reflecting the urgent need for robust detection systems. The financial implications of these fraudulent claims are substantial, with estimates suggesting that healthcare fraud costs the industry billions annually. Consequently, healthcare providers and insurers are increasingly investing in advanced fraud detection technologies to mitigate these losses and enhance operational efficiency.
Technological Advancements in Detection Systems
Technological advancements play a crucial role in shaping the Global Medical Payment Fraud Detection Market Industry. Innovations such as artificial intelligence and machine learning are being integrated into fraud detection systems, enabling more accurate identification of suspicious activities. These technologies can analyze vast amounts of data in real-time, significantly improving the efficiency of fraud detection processes. As the market is projected to grow to 14.7 USD Billion by 2035, the adoption of these advanced technologies is likely to accelerate, providing healthcare organizations with the tools necessary to combat increasingly sophisticated fraudulent schemes.
Regulatory Compliance and Government Initiatives
Regulatory compliance and government initiatives are pivotal in driving the Global Medical Payment Fraud Detection Market Industry. Governments worldwide are implementing stricter regulations to combat healthcare fraud, which necessitates the adoption of effective fraud detection solutions. For instance, the Centers for Medicare & Medicaid Services in the United States has introduced various programs aimed at reducing fraud and abuse in healthcare. These initiatives not only promote accountability but also encourage healthcare providers to invest in fraud detection technologies, thereby expanding the market. The anticipated CAGR of 21.29% from 2025 to 2035 underscores the growing importance of compliance in this sector.