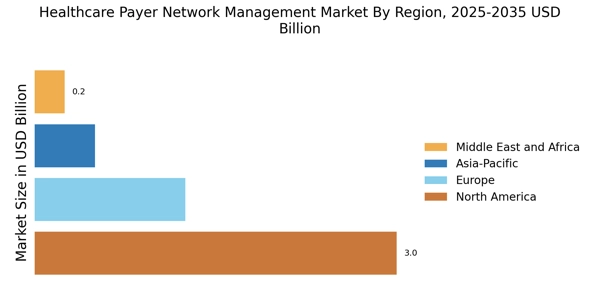
Healthcare Payer Network Management Market Summary
According to Market Research Future analysis, the Healthcare Payer Network Management Market Size was valued at USD 4.974 Billion in 2024. The Healthcare Payer Network Management industry is projected to grow from USD 5.646 Billion in 2025 to USD 20.07 Billion by 2035, registering a CAGR of 13.52% during the forecast period (2025–2035). North America led the market with over 60.31% share, generating around USD 3 billion in revenue.
The Healthcare Payer Network Management Market is expanding due to the growing complexity of healthcare systems and increasing demand for efficient provider network coordination. Key trends include adoption of digital health management platforms, integration of data analytics for provider performance monitoring, and rising focus on cost optimization and value-based healthcare delivery.
The European Centre for Disease Prevention and Control emphasizes that strong healthcare information systems and coordinated provider networks are essential for effective disease monitoring and public health response, reinforcing demand for digital healthcare management platforms.
Key Market Trends & Highlights
The Healthcare Payer Network Management Market is experiencing a transformative shift towards data-driven and patient-centric approaches.
- The market is witnessing an increased focus on data analytics to enhance decision-making and operational efficiency.
- Integration of technology solutions is becoming prevalent, facilitating seamless network management and improved service delivery.
- Value-based care is gaining traction, reflecting a broader industry shift towards patient outcomes and cost-effectiveness.
- Rising demand for cost efficiency and regulatory compliance are driving growth, particularly among commercial payers in North America and government payers in the Asia-Pacific region.
Market Size & Forecast
| 2024 Market Size | 4.974 (USD Billion) |
| 2035 Market Size | 20.07 (USD Billion) |
| CAGR (2025 - 2035) | 13.52% |
Major Players
Companies such as UnitedHealth Group (US), Anthem (US), Aetna (US), Cigna (US), Humana (US), Centene Corporation (US), Molina Healthcare (US), WellCare Health Plans (US), Blue Cross Blue Shield (US) are some of the major participants in the global market.
.png?v=1777014025)