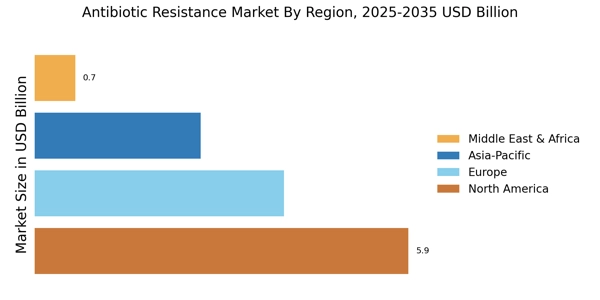
North America : Leading Innovation and Research
North America leads in the Antibiotic Resistance Market Size, accounting for over 45% of the global revenue in 2024. The region benefits from robust healthcare infrastructure, significant R&D investments, and stringent regulatory frameworks that promote innovation. The increasing prevalence of antibiotic-resistant infections drives demand for new therapies and diagnostics, supported by government initiatives aimed at combating this public health crisis.
The United States is the primary contributor to this market, with key players like Pfizer, Merck & Co, and Johnson & Johnson leading the charge. The competitive landscape is characterized by ongoing collaborations between pharmaceutical companies and research institutions, fostering the development of novel antibiotics and alternative therapies. The presence of advanced healthcare facilities further enhances the region's capability to address antibiotic resistance effectively.
Europe : Collaborative Regulatory Frameworks
Europe Antibiotic Resistance Market was valued at USD 2.91 billion in 2024, making it the second-largest regional market with a 30% share. Leading countries in this market include Germany, France, and the UK, contributing to the germany antibiotic resistance market, france antibiotic resistance market, uk antibiotic resistance market, italy antibiotic resistance market, and spain antibiotic resistance market growth outlook within the broader regional landscape.
The European Medicines Agency (EMA) plays a crucial role in facilitating the approval of new antibiotics and promoting responsible use of existing ones, thereby enhancing public health outcomes. Leading countries in this market include Germany, France, and the UK, where major pharmaceutical companies like AstraZeneca and GSK are actively engaged in research and development.
The competitive landscape is marked by a focus on innovation, with increasing investments in biotechnology and partnerships aimed at discovering new therapeutic options. The European market is characterized by a strong emphasis on sustainability and responsible antibiotic use, aligning with global health initiatives.
Asia-Pacific : Emerging Market Potential
Asia-Pacific is witnessing rapid growth in the antibiotic resistance market, holding approximately 20% of the global market share. Countries like China and India are at the forefront, driving expansion in the india antibiotic resistance market and south korea antibiotic resistance market through improved healthcare investments. China is the largest market in the region, with significant investments from both government and private sectors in combating antibiotic resistance.
The competitive landscape features a mix of local and international players, including Novartis and Bayer, who are focusing on developing innovative solutions tailored to regional needs. The growing prevalence of resistant infections is prompting a surge in demand for effective antibiotics and alternative treatments, making Asia-Pacific a key area for future growth.
Middle East and Africa : Challenging Healthcare Landscape
The Middle East and Africa region is gradually emerging in the antibiotic resistance market, accounting for approximately 5% of the global market share, with increasing activity observed across the gcc antibiotic resistance market. The growth is driven by increasing awareness of antibiotic resistance and the need for improved healthcare systems. However, challenges such as limited access to healthcare and inadequate regulatory frameworks hinder rapid progress.
Governments are beginning to recognize the importance of addressing antibiotic resistance as a public health priority, leading to the development of national action plans. Countries like South Africa and the UAE are taking the lead in implementing strategies to combat antibiotic resistance, with support from international organizations.
The competitive landscape is still developing, with a focus on partnerships between local and global pharmaceutical companies. Key players are beginning to invest in research and development to address the unique challenges faced in this region, paving the way for future advancements in antibiotic solutions.